The pancreas
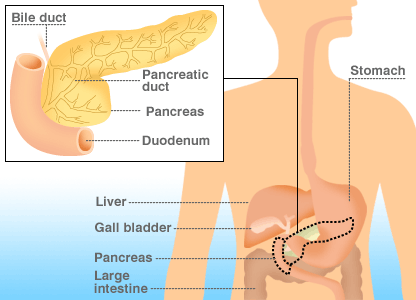
The pancreas is about 6-inch gland located below the liver, between stomach and spine. The pancreas is made up of 3 parts: a “head” that is tucked into the duodenum (the upper part of the small intestine); a flattened, longer “body;” and a “tail” that is connected to the spleen. The pancreas has dual roles; it is an organ of the digestive system and of the endocrine (hormonal) system. The pancreas adds its own digestive juices and enzymes to the food, via a small duct attached to the duodenum. This process is said to belong to the ‘exocrine pancreas’. The pancreas also produces the hormone insulin, which helps to control the amount of sugar in the blood. This is the role of the ‘endocrine pancreas’.
Pancreas has got the peculiarity of auto digestion ( self destruction by its own secretion). Surgeries in this organ are difficult. May lead to leakage of pancreatic juice, pancreatitis & pancreatic fistula. Techniques should be meticulous and well planned to minimize the risk of complications.Pancreatitis
An inflammation of the pancreas is called pancreatitis. Pancreatitis can either be acute (a sudden, sharp, and/or severe attack) or chronic (recurring and/or lasting for a long period of time). When the pancreas is inflamed, digestive enzymes become activated while still inside the pancreas, which can cause the pancreas to begin “digesting” its own tissues ( auto digestion).Acute Pancreatitis.
This is sudden inflammation of the pancreas. In over half the cases it is caused by a gallstone passing from the gallbladder, through the bile duct and temporarily blocking the exit from the bile duct and pancreatic duct.(upper picture)
This causes obstruction of the pancreas, and may allow bile to reflux into the pancreatic duct (lower picture – close up).
About a quarter of cases of acute pancreatitis are caused by drinking too much alcohol and there is a long list of other rare causes including a wide variety of prescription medications, virus infections including mumps, hypothermia and (in the tropics) scorpion stings. Most attacks of pancreatitis (about 80%) are relatively mild and settle spontaneously over a period of 4 or 5 days. The usual symptoms of pancreatitis are severe pain in the upper part of the abdomen, often going into the back, and occasional vomiting.
If the pancreatitis is caused by gallstones it is essential to ensure that appropriate treatment to prevent a further attack is completed before the patient leaves hospital. This will usually be either by a laparoscopic Cholecystectomy (removal of the gallbladder) or an endoscopic procedure (ERCP and sphincterotomy) which opens the lower end of the bile duct and allows any stones in the duct to pass easily without causing obstruction .Anyone who has alcohol-associated pancreatitis is at risk of further attacks should abstain from alcohol indefinitely
About 1 in 5 people develop serious complications, either in or around the pancreas, or involving other systems in the body especially the lungs and the kidneys. These systemic complications are due to an excessive inflammatory reaction to the damage in the pancreas. At the moment treatment for this phase of the illness is supportive, and may require transfer to the intensive care unit if the condition is serious.
Necrosis of the pancreas (necrotizing pancreatitis) :
The local complications during pancreatitis due to severe inflammation leading to necrosis of pancreatic tissue and the surrounding fatty tissue. Patients with necrosis usually have systemic complications as well and often need to stay in intensive care or high dependency unit for several days. The necrotic tissue may become infected and when this happens the only solution is to remove the infected necrotic tissue (Necrosectomy).It might also need fixation of a lavage system by drainage tubes (closed cavity lavage) for continuous irrigation and removal of ongoing necrosed tissues. It may take long time
Patients with pancreatic necrosis should be treated by a specialist hepato- bilary- pancreatic surgery centre with intensive care and other facilities.
Chronic pancreatitis.
This is the recurring inflammation and progressive damage in the pancreas. Symptoms usually include abdominal pain particularly in the upper abdomen, and often going into the back. Other symptoms may be jaundice, weight loss, changes in the bowel motions including frequency, and loose pale stools
Finally, it must be recognized that chronic pancreatitis is an ongoing disease that does not have a simple treatment or cure, and frequently represents a process of remissions and relapses requiring interventions and problem solving.
The commonest cause of chronic pancreatitis is long term alcohol consumption. However there are many other causes, and in at least a quarter of patients no known cause is found. The rare causes include exposure to industrial toxins. Congenital variations and stricture (s) in the pancreatic duct system are the main cause. It might also associated with stone (s) in the pancreatic duct system and pancreatic parenchyma.( pancreatolithiasis)
Most patients with chronic pancreatitis require multidisciplinary management . This includes replacement of pancreatic enzymes (enzyme supplements) attention to nutrition with a proper balanced diet. The most important aspect of treatment for many patients is pain control.
Medical management is avoidance of any precipitating factors. For this reason any patient with chronic pancreatitis is advised strongly to avoid alcohol completely..
Surgical treatment: There are many reasons for surgical treatments in chronic pancreatitis. Surgery may be required to deal with stricture of pancreatic duct, removal of stone (s), relieve of pain from the pancreas, or to treat complications such as jaundice or pseudocysts.
Pancreatic stone: (pancreatolithiasis)
Pancreatic duct stones usually develop from cholesterol or bile salts and can block the flow of digestive enzymes from the pancreas to the small intestine. It is invariably associated with chronic pancreatitis and ductal stricture. The calculi form in the major and minor (second generation) pancreatic ducts. Commonly associated with diabetes (>85%) and malnutrition(>73%) and steatorrhea ( about 12%) Pancreatolithiasis associated with pancreatic cancer in 3% to7% , in high endemic areas it is approximately 28%.
When the stones block the pancreatic duct, which connects the pancreas with the small intestine, the pancreas loses its ability to release digestive enzymes; the secretion of hormones that regulate blood sugar levels can also be affected.
Stone(s)in the pancreas is one of the common pancreatic diseases which need surgical intervention
In addition to the stones that form in the pancreas, stones that form in the gallbladder (gallstones) may become lodged in the common bile duct, which merges with the pancreatic duct. If either type of stone blocks the pancreatic duct pancreatic enzymes can back up inside of the pancreas, resulting in inflammation and pancreatitis.
Causes – Pancreatic duct stones often result from pancreatitis associated with alcohol abuse, hyperparathyroidism or Islet cell tumors.
Symptoms – Pancreatic duct stones often occur during episodes of pancreatitis. The signs and symptoms of acute pancreatitis may vary by person but is most commonly characterized by:
Abdominal pain that is felt in the upper left side or the middle of the abdomen. The pain may be worse after drinking or eating (especially foods that have a high fat content) or when lying on your back, and may radiate to the back or below the left shoulder blade.other symptoms are , Vomiting ,Jaundice, Clay-colored stools
Diagnosed by abdominal Xray, Abdominal Ultrasound ,Endoscopic Retrograde Cholangiopancreatography (ERCP and Endoscopic Ultrasound (EUS)
CT scan is of great value in determining characteristics and locations of pancreatolithiasis associated with pancreatic cancer
Treatment – Effective treatment requires that the stones to be removed. Small stones can be removed by endoscopy, choloangiopancreatography (ERCP); larger and multiple stones require surgery.
Pancreatolithotomy (removal of stone(s) plus side-to-side pancreaticojejunostomy (anastmosis between pancreatic duct and small bowel) is the best choice for the treatment of pancreatolithiasis.. Biopsy of pancreas is mandatory to exclude the possibility of associated pancreatic cancer. Pancreatic stone with extensive pancreatic fibrosis or damage may need resection in the form Whipple’s procedure or distal pancreatectomy. For patients with pancreatolithiasis associated with pancreatic cancer, surgical treatment should follow the principles of individualized therapy.
Pancreatic cysts:
A pancreatic cyst is a closed sac lined with epithelium and located on or within the pancreas. Pancreatic cysts contain a pool of pancreatic fluid or semisolid matter made up of debris or destroyed tissue.
They can range from benign pseudocysts (see below) to malignant cysts (cancerous and spreading.) The cause of a particular pancreatic cyst is often unknown. Some pancreatic cysts result from certain rare diseases, such as von Hippel-Lindau disease (a genetic disorder).
Pancreatic Pseudocyst:
Are the most common pancreatic cystic lesions (about 75% to 80% of all pancreatic cystic lesions) Are health problems caused by acute or chronic pancreatitis, It is caused by blockage in the pancreatic ductal system. It is usually round or oval in shape and benign (non-cancerous).
Pseudocyst. usually resolve spontaneously by gradual absorption of the fluid, but sometimes, especially if there is a communication with the pancreatic duct, the cyst will persist and may cause symptoms by pressure on other organs or by infection and causing septicemia. Such symptomatic Pseudocyst need treatment. This is usually done by removal of contents and internal drainage of cyst with bowel by surgery . The surgery involves connecting the wall of the cyst to either the wall of the stomach or an adjacent loop of bowel and forming a permanent join that allows the fluid to drain into the stomach or intestine Sometimes endoscopic internal drainage by placement of stent ( tube) between cyst cavity and stomach.is helpful.
Complications of pancreatic pseudocysts?
Many complications can come from pancreatic cysts/pseudocysts, including:
Infection, which can sometimes lead to pancreatic abscess
Pseudocyst rupture (breaking open) or hemorrhage (bleeding), which can happen without warning and which can be life-threatening
Biliary complications, which can occur when a large cyst blocks the common bile duct, causing skin, mucous membranes, and whites of the eyes to appear yellow (obstructive jaundice)
Portal hypertension, or high blood pressure of the splenic vein/portal vein, which requires How are
pancreatic cysts and pseudocysts treated?
Most pseudocysts resolve themselves without treatment, over time. However, when symptoms become persistent, complications emerge, or cysts become larger than 6 centimeters in size, drainage is indicated.Pancreatic cystic Tumors:.
Cystic tumors of the pancreas are less frequent than solid lesions and are often detected incidentally, as many of these lesions are small and asymptomatic. However, they may be associated with pancreatitis or have malignant potential. With advancements in diagnostic imaging, cystic lesions of the pancreas are being detected with increasing frequency. Many lesions can cause a pancreatic cyst, most being non-neoplastic while approximately 10% are cystic tumors, ranging from benign to highly malignant tumors. Even small cystic lesions of the pancreas appear to have the potential to progress to malignancy , and at least need follow-up with repeat imaging.
A presumptive diagnosis of pseudocyst based on imaging appearance alone can cause a diagnostic error, and neoplastic cysts of the pancreas are particularly susceptible to this misdiagnosis, which can result in inappropriate treatment. Cystic tumors of the pancreas are formed by serous or mucinous structures showing all stages of cellular differentiation
Cystic pancreatic tumors can be subdivided into peripheral (serous cystadenomas, mucinous cystic tumors, solid and papillary epithelial neoplasms, cystic islet cell tumors), On the basis of imaging criteria alone, it can be very difficult to differentiate non-tumoral cystic lesions from neoplastic ones. The management of these patients are complex, and it is important to correlate imaging findings with knowledge of the patient’s symptoms and of the natural history and predictors of malignancy in pancreatic cysts.
Cystic tumours of pancreas needs evaluation to differentiate from its counter part pseudocyst first. If true cyst then to differentiate benign from malignant cystic lesion.(cancer). Imaging characteristics, tumour marker, per operative findings, cytology of cyst fluid, Frozen section of the cyst wall are the guideline for decision making about the nature of the lesion. Malignant ( cancer) lesion needs adequate resection of the affected part of the pancreas. Benign lesion can be treated by internal drainage to bowel. Precaution to be taken that a cancerous lesion should never be left in the pancreas or drained to bowel
Solid pseudopapillary tumor
Solid pseudopapillary tumor (SPT) is the least frequent cystic tumor of the pancreas whose origin is still uncertain. It has a low malignant potential and a favorable prognosis. It may affect any age, but most often affects young women in their 30s . Clinically it is fairly nonspecific, with abdominal pain as the main symptom, sometimes together with a palpable mass. The low malignant potential of the lesion is demonstrated by its large size at the time of the diagnosis . The tumor appears as a round, well-encapsulated mass . The content of the lesion is solid with a variable amount of necrosis or hemorrhage, responsible for its frequent cystic appearance. . After contrast agent administration the solid component of the tumor appears well vascularized ,cyst s appear as hypodense areas.
This tumor should be treated by adequate pancreatic resection, which can offer cure in most circumstances.
Pancreas Cancer:
Cancers of the pancreas are the 4th most common cause of cancer death world wide , incidence of pancreatic cancer increases with age. More in male then female The vast majority of patients are aged between 50 and 80 years of age .
The only known risk factor is smoking. Diabetes is not known to increase the risk of pancreatic cancer. Dietary factors such as alcohol and fat have been implicated but not proven as yet to cause pancreatic cancer.
The symptoms of pancreatic cancer are generally vague and non-specific. Weight loss is one of the earliest symptoms Abdominal pain is not uncommon late in the disease. Another late symptom is jaundice, or yellowness of the whites of the eyes
If pancreatic cancer is suspected, the initial diagnostic test would be a CT or computerized scan of the abdomen. The CT scan is able to detect any pancreatic mass greater than 2cm in 95% cases. Smaller cancers are more difficult to detect. Magnetic resonance imaging (MRI) scans can visualize the pancreas and the ducts in the pancreas. This can be particularly useful when planning surgery.
Another procedure that is often done is an endoscopic retrograde cholangiopancreaticography (ERCP) which involves using a fiberoptic scope to look into the stomach and small intestine where the ducts of the pancreas drain into duodenum. The tumour can also be biopsied during this procedure. If a blockage of the ducts is seen, a small plastic tube, called a stent, can be placed during this same procedure to release the block.
Sometimes, when a biopsy cannot be obtained via ERCP, a percutaneous biopsy of the pancreatic lesion is performed to obtain tumour tissue for diagnosis. This involves inserting a needle through the abdominal wall to the pancreas under CT or ultrasound guidance.
Treatment of Pancreas Cancer
Surgery continues to be the treatment of choice for pancreatic cancer. Early diagnosis increases the resection rate The nature of surgery depends on the site of pancreatic cancer.
Whipple’s Procedure:
If the cancer in the ampullary , periampullary or head region ( ie Right side), then the standard surgery is partial pancreato duodenectomy popularly known as Whipple’s Procedure. It involves resection of portions of multiple structures like distal part of stomach, head of the pancreas, gall bladder, distal bileduct, duodenum and part of proximal small bowel leaving behind the major blood vessels. After removal of these structures the anatomical and functional integrity is restored by anastmosis of bowel with the structures like pancreas ( pancreato jejunostomy), bileduct ( hepatico jejunostomy), Stomach ( gastro jejunostomy) and bowel with bowel ( entero- enterostomy). .
Distal pancreatectomy: Tumours in the body and distal part ( ie Left side) of pancreas needs distal pancreatectomy This involves dividing the left side of the pancreas to remove areas of disease in the tail and body of the pancreas. This operation is used more often with islet cell tumors found in the tail and body of the pancreas.. The tail of the pancreas lies directly in front of the blood vessels to the spleen. Sometimes it become difficult to separate the blood vessels of the spleen from the tumor, in that situation spleen also must have to be removed. The spleen is an important part of the immune system; Splenectomy causes increase chance infection of some of the organism. Prophylactic vaccine against infection is given prior to its removal
Middle pancreatectomy:.If the tumor in the pancreas is in the middle part, then middle portion of the pancreas removed. This is a pancreatic parenchyma preserving procedure. The proximal part with head of the pancreas and also the distal part. is preserved. Duct of the proximal part closed and the distal part anastomosed with bowel ( pancreato jejunostomy) for drainage of pancreatic juice.
Pancreatic bypass Procedure :
It is known that only 18% to 20% pancreas cancers are respectable. Most patients are not candidates for curative surgery because of the advanced stage of disease when diagnosed. Even if curative surgery is not possible, bypass procedures performed for patients with blockage of the bile duct (causing jaundice) or duodenum caused by pancreatic tumours that cannot be removed during the time of surgery .It is performed to improve the patient’s quality of life.
Prognosis of Pancreas Cancer:
Even with curative surgery, about half of patients with pancreatic carcinoma survive between 2 to 3 years. The chance of surviving to 5 years after curative surgery is about 20%.